Hospital acquired infection
Few statistics related to Hospital-acquired infection (HAI):
- Anyone admitted to a hospital has a 5 percent chance of contracting an HAI.
- Your length of stay in the hospital increases by 17.6 days if you get an HAI.
- 1.7 million people per year get an infection during a hospital stay.
- 9.4% of total inpatient costs are HAI-related.
- HAIs kill more people each year than breast cancer and prostate cancer combined.
- Antibiotics are often used to treat HAI and increases the risk for the spread of multi-resistant bacteria.
Hospital Acquired Infection also known as a nosocomial infection, is an infection that is acquired in a hospital or other health care facility. To emphasize both hospital and non-hospital settings, it is also termed as a health care–associated infection (HAI). These infections are a result of germs entering your body during medical care. Bacteria, virus and fungi are some of the agents of nosocomial infections.
Symptoms of HAIs vary by type. The most common types of HAIs are:
- Urinary tract infections (UTIs)
- Surgical site infections
- Gastroenteritis
- Meningitis
- Pneumonia
The symptoms for these infections may include:
- Discharge from a wound
- Fever
- Cough, shortness of breathing
- Burning with urination or difficulty urinating
- Headache
- Nausea, vomiting, diarrhea
Anyone admitted to a healthcare facility is at risk for contracting a HAI while the risk may also depend on:
- Your hospital roommate.
- Age factor, especially if you’re more than 70 years old.
- How long you’ve been using antibiotics
- Prolonged ICU stay.
- If you’ve experienced any trauma or shock.
- Your compromised immune system.
Where there is a problem, there is also a cure. One must follow standard safety measures to minimize the infection:
- Wash hands with chlorhexidine or 70% isopropyl hand-sanitizer or warm soap and water.
- Disinfect and keep the surfaces clean.
- Prevent patients and attendants from walking barefoot.
- Keep surrounding clean and spillage-free.
- Provide infection control education.
- Food and beverages must be kept at proper temperatures in order to avoid spoilage.
Above mentioned cures along with well-designed products can save a patient from infections that might come his/her way during hospitalization.
Romsons has a specialized range of products with closed system that help in maintaining a closed environment for the patient, thus, reducing the chances of infection.
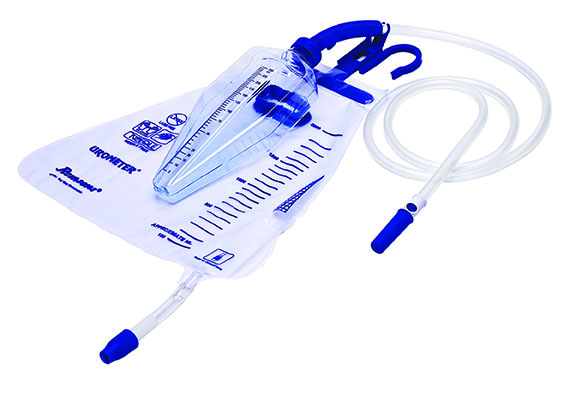
Urometer Plus (hourly urine output bag) are designed to measure the patient’s accurate urine output and its needle free sampling port helps in reducing the chances of Catheter-Associated Urinary Tract Infection (CAUTI).
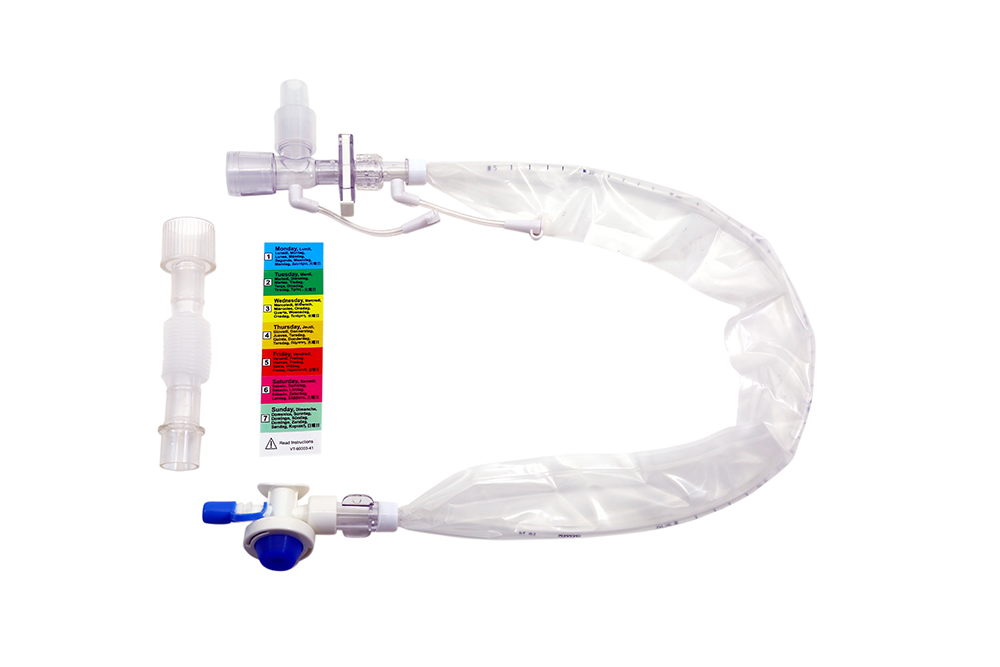
Close Suck Cath (Closed Suction Catheter) which is used for suctioning the ventilated patients in the closed environment, reduces the chances of nosocomial infection and hypoxia, and can be used upto 72 hrs continuously.

Succor (Sub-glottic endotracheal tube) has been specially designed to aspirate the secretions from sub-glottic region, above the cuff that helps in reducing the chances of Ventilator Associated Pneumonia (VAP) drastically.

Exteena (needle-free devices) specially designed to reduce the chance of Catheter-related bloodstream infection (CRBSI).
Case Study
Hospital Associated infections (HAI) are very common in Intensive Care Units (ICU) and are usually associated with use of invasive devices in the patients. This study was conducted to determine the prevalence and etiological agents of HAI in a Surgical ICU and to assess the impact of these infections on ICU stay and mortality.
This retrospective, observational study was conducted in a 12-bed ICU. All patients who were admitted to the ICU from January – November, aged 18 to 90 years, developed an HAI. On completion of the same, it was found that the most common type of HAI was surgical site infection (SSI), followed by ventilator-associated pneumonia (VAP), catheter-related blood stream infection (BSI) and catheter-associated urinary tract infection (UTI). The most common etiological agent was found Pseudomonas aeruginosa with SSI infected patients.
The second most common HAI was VAP also with P. aeruginosa followed by BSI which was also associated with the same pathogen and also Enterococcus faecalis, and Klebsiella pneumoniae as the most common etiological agents causing these infections.
It has been found that HAI among the study population were predominantly caused by gram- negative pathogens, including P. aeruginosa, K. pneumoniae, and E. coli.
The most effective and important interventions to prevent HAI are active surveillance, regular infection control audits, rational and effective antibacterial therapy, and general hygiene measures.
